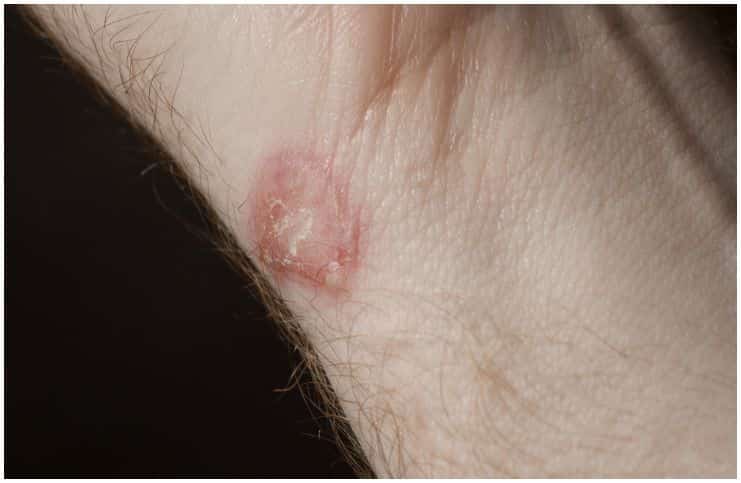
Nummular Eczema vs Ringworm – Symptoms, Causes, Diagnosis, Treatment, Prevention:
Nummular Eczema
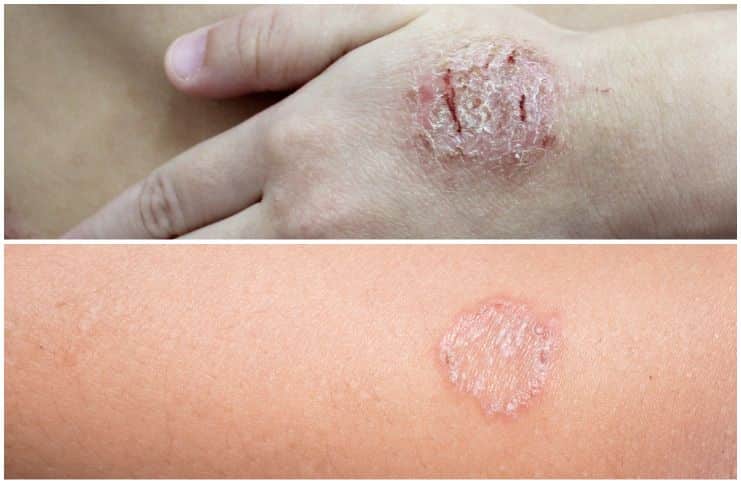
Nummular eczema, also called discoid eczema, is a rare skin condition characterized by coin-shaped spots on the skin. Many times it starts on the back of your hips, back of your hand, and legs.
This skin condition tends to be chronic, with periods when it gets much better or worse.
It commonly occurs in the winter and usually becomes worse at that time.
The word ”nummular” is Latin for “resembling coins,” and it was first described in 1857 by Deverigie.
The prevalence is around 2 per 1,000 people. When women get it, they are generally younger. Men usually have their first outbreak between 55 and 65 years of age.
Moreover, in males over the age of 50 years, there is a strong association with chronic alcoholism. Interestingly, men get it more often than women.
Symptoms
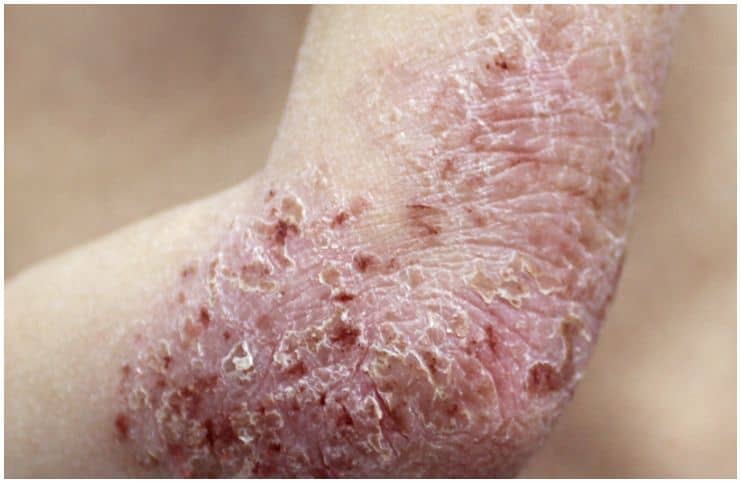
- Skin inflammation or redness;
- Coin-shaped skin lesions, which are scaly and dry, appear on the legs and arms. At times, these lesions may cause a burning sensation or itchiness.
Causes
The reason for this skin condition is unknown. However, it may occur as a result of having unusually dry skin.
Also, infection with Candida or Staphylococcus aureus (a Gram-positive, round-shaped bacterium) may play a role.
Additionally, recent studies have associated allergic reactions caused by cobalt, nickel, chromate, and fragrance as possible causes of this condition.
Moreover, injury to the skin or insect bites can trigger an outbreak of skin conditions in some people. Occasionally, certain prescription medicines (drugs used to treat hepatitis C infection, called ribavirin and interferon) can trigger it in some people.
Alcohol consumption can also be implicated in the development of this condition, making it vital that you eliminate it from your diet, according to a 2011 study conducted by Well Cornell Medical College, Texas.
Diagnosis
It is clinically based on the characteristic appearance and distribution of the skin lesions.
Tests for fungi and bacteria may be done to rule out infection. However, patch tests are frequently negative in people with this problem.
Treatment
It is focused on preventing future flare-ups, and when a flare-up does occur, immediately treating the symptoms of the rash.
Usually, treatment includes antihistamines, such as – Benadryl, that can be useful in the reduction of itchiness. These itchy sensations can interfere with sleeping; hence, it is recommended that antihistamines are applied before going to sleep.
In more severe cases, steroid tablets may be needed.
Due to the fact that they are very strong, they should not be used in some parts of the body, like – the armpits, face, and other areas where the skin is too sensitive.
If infection occurs, an antibiotic will be necessary (most often flucloxacillin). Occasionally, this skin condition clears entirely on oral antibiotics, only to recur when they are stopped.
Prevention
Avoid detergents and soaps, such as – bubble baths, liquid soaps, wet wipes, and shower gels – even if these do not obviously irritate the skin. Also, you should use an emollient instead of soap.
Avoid exposure to irritants, including – detergents, cleaners, and chemicals.
If you have sensitive skin, then it is essential that you prevent hurting yourself (cuts, bruises, or skin scrapes).
Keeping your fingernails short and your hands clean may help lower the risk of skin damage from accidental scratching.
Fabrics like – synthetics and wool may irritate the surface of the skin, and these should be replaced with light cotton garments.
In some cases, food additives can also irritate the skin. Furthermore, certain foods, like – peanut butter, eggs, and fish, are known to trigger this condition.
Ringworm
Ringworm, also known as tinea corporis, is actually a skin infection usually caused by one of three species of fungus: Microsporum, Trichophyton, and Epidermophyton.
There is no actual ”worm” involved.
The infection may affect the skin of the feet, scalp, beard, groin, or other areas and can spread via clothing, skin-to-skin contact, or surfaces where the fungus lives, like – showers or locker rooms.
In the United States, the infection accounts for about 90% of fungal infections of the skin in children under age 10.
Symptoms
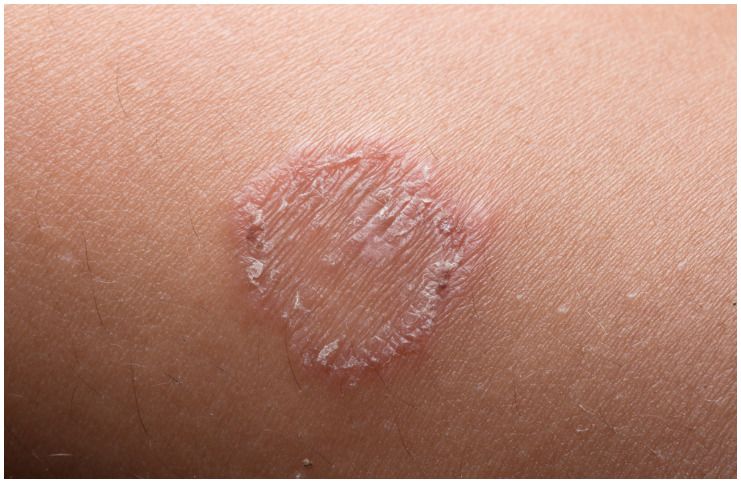
- itchy, scaly, and inflamed skin;
- hair loss in the affected area;
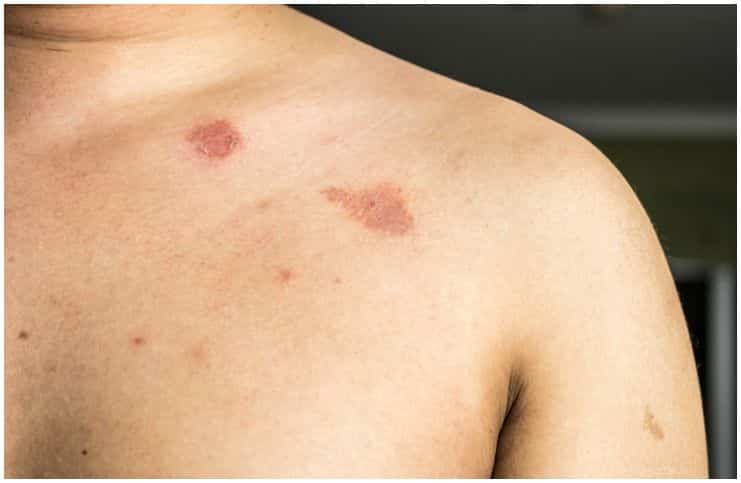
- a silvery rash or ring-like red on your skin – your skin will look healthy inside but irritated and red around the ring.
Note – lesions usually appear 10 to 28 days after exposure to the fungus.
Causes
It is caused by mold-like parasites that live on the cells in the outer layer of your skin.
Diagnosis
This condition can be diagnosed by your GP after asking whether you have other related symptoms and examining your skin.
Treatment
It can be treated with antifungal medications used either orally or topically.
Without treatment, the rash tends to grow slowly and cover a larger area. Also, you can infect other areas of your body.
Note – if the rash does not clear after you have tried different topical antifungals belonging to the allylamine class (terbinafine) or azole class (like – miconazole and clotrimazole), or if the infection is widespread, you may require prescription antifungal pills, such as:
- Lamisil or Terbinex (terbinafine);
- Gris-PEG (griseofulvin);
- Sporanox or Onmel (itraconazole);
- Diflucan (fluconazole).
If you are pregnant or nursing, you should make an appointment with your healthcare specialist to find out the best method to treat this condition since antifungals may not be suitable for you.
Prevention
Avoid tight pants, underwear, and pantyhose, and wear loose-fitting cotton clothing.
Keep shared areas clean, particularly in childcare centers, schools, gyms, and locker rooms. Wash your hands frequently to avoid the spread of infection.
Change your underwear and socks at least once a day. Keep your skin dry and clean.
After being exposed to places where the potential of being infected is high, it is recommended to wash with soap which contains tea tree oil.
Stay away from infected animals and get your pets checked for ringworm by your vet. On domestic animals, this condition looks like a patch of missing fur.
If you’re a professional athlete involved in close contact sports, you should shower immediately after your practice session.
Change your sheets once every seven days and wash them in hot water, at least 140 degrees Fahrenheit.
Wear sandals or slippers in showers, locker rooms, and public bathing areas.
Bottom Line – Nummular Eczema vs Ringworm
Ringworm isn’t severe (but highly contagious and is easily spread among people) and is usually easily treated using creams. Nevertheless, nummular dermatitis is long-lasting, with symptoms leaving and recurring again indefinitely.
READ THIS NEXT:
Hydrogen Peroxide vs Rubbing Alcohol
Pros And Cons Of Being A Vegetarian
Dangers And Side Effects Of Donating Plasma Regularly
References https://www.ncbi.nlm.nih.gov/pubmed/21611681 http://www.nhs.uk/Conditions/