Folliculitis vs Herpes – Differences in Symptoms, Causes, and Treatment:
Folliculitis
It is an inflammation affecting the hair follicles, which are the hair-producing pores on your skin.
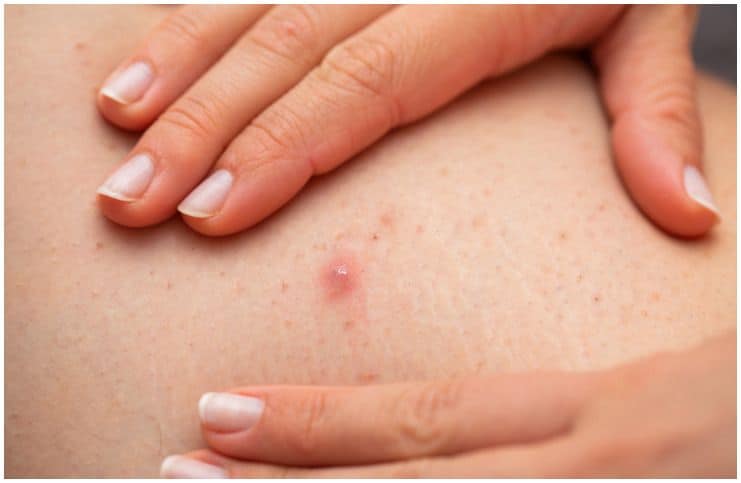
The infection presents itself as a small white or red pimple with a strand of hair in the middle of the pus. It may look like a rash or acne.
This inflammation can occur almost anywhere on the skin; however, it is most typically found on the neck, buttocks, thighs, or armpits.
It does not occur on the soles or palms or on mucous membranes because they have no hair follicles.
Symptoms
Common symptoms include:
- large areas of red, swollen skin which may leak pus;
- blisters which break open, ooze, and become crusty;
- groups of small red bumps, such as – pimples, some with whiteheads on them.
Causes
There are many causes for this condition, including:
- blockage of hair follicles by oils, creams, or ointments;
- irritation from tight clothing or sporting equipment rubbing against the skin;
- infections by Staphylococcus aureus or other bacteria;
- exposure to hot water for long periods of time, such as – a Jacuzzi or a hot tub;
- a weakened immune system caused by conditions like – cancer or HIV;
- skin-clogging substances, like – motor oil and tar;
- excessive sweating due to overactivity of the sweat glands;
- irritation from plucking, shaving, or waxing hair.
Diagnosis
The diagnosis of this condition is usually based on the appearance of the skin.
Sometimes, a microbial culture of pus from the pustules is taken to help detect the infection.
Treatment
This condition usually clears without any treatment within 7 to 10 days. However, more severe infections may cause permanent hair scarring or loss, and medication may be required to kill the pathogenic bacteria.
Your doctor may prescribe:
- antihistamines or nonsteroidal anti-inflammatory drugs to relieve pain or itching;
- antifungal medications or topical/oral antibiotics to treat the cause of the infection.
Folliculitis that is produced by poor shaving technique can be treated with weak topical steroids.
Hair removal laser treatments may be used for resistant and recurrent cases, particularly on the legs.
Aloe vera is a natural home remedy for this condition due to its anti-inflammatory and antibacterial attributes, which help relieve the itching and burning.
Prevention
Prevention methods include:
- stay cool to avoid sweating;
- avoid friction from tight clothing, such as – blue jeans, in the affected area;
- don’t scratch the affected area, and wash your hands thoroughly after contact with an infected individual;
- have a diet rich in omega-3 fatty acids (walnuts, chia seeds, flax seeds, red kidney beans);
- shave in the direction of hair growth with shaving cream or gel;
- avoid public hot tubs or spas;
- take a daily shower or bath and change bedding, towels, and clothes often;
- don’t wax, shave, or pluck the area until symptoms have cleared.
Herpes
It is an infection caused by HSV (herpes simplex virus).
There are two types of HSV:
HSV-1 (herpes type 1, or oral herpes) – over 3.7 billion people under age 50 have HSV-1 infection globally. Although HSV1 infection can occur at any age, most individuals get their first infection in early childhood.
HSV-2 (herpes type 2, or genital herpes) – over 417 million people aged 15-49 worldwide have the HSV-2 infection. Also, an estimated 1 out of 9 men aged 14 to 49 years in the United States has genital herpes.
Symptoms
HSV-1 is responsible for fever blisters and cold sores, usually occurring around the mouth.
Also, HSV-1 may infect the eye, causing visual impairment and corneal ulcers.
Some people may also experience some unusual redness and swelling in the affected area.
HSV-2 can cause small blisters which burst to leave red, open sores around the genitals, anus, buttocks, or thighs. In women, it may cause vaginal discharge.
Note – some individuals who are infected with HSV-2 but don’t have any symptoms still have active forms of the virus detected in their genital tract.
Moreover, both types of virus can make sores pop up on and around your vagina, vulva, cervix, penis, anus, scrotum, inner thighs, butt, lips, throat, mouth, and eyes.
Causes
HSV-1 can be spread through kissing or sharing objects, like – eating utensils or toothbrushes. Because it is highly contagious, a majority of the population is infected with at least 1 herpes subtype of HSV-1 before adulthood.
HSV-2 can be spread through vaginal, anal, and oral sex with someone who has a genital HSV-2 infection.
Diagnosis
This infection can be diagnosed by scraping the base of the cold sore and examining cells under the microscope.
Treatment
Symptoms clear in 7-10 days, with or without treatment, but the virus will remain in a dormant state in the body.
Recurrent and severe infections may need ongoing suppression therapy with oral antiviral medication to prevent outbreaks.
These treatments include:
- penciclovir (Denavir)
- famciclovir (Famvir)
- valacyclovir (Valtrex)
- acyclovir (Zovirax)
Also, treatments with vitamin C, lysine, zinc, adenosine monophosphate, vitamin E, and lemon balm are effective.
Prevention
Prevention methods include:
- do not share drink or food containers;
- do not perform oral sex if cold sores are present;
- do not kiss on or near the cold sore;
- don’t wet contact lenses with spit;
- follow good hand washing techniques;
- when possible, cold sores should be covered with a dressing;
- always use condoms and dental dams during anal, oral, and vaginal sex.
Bottom Line – Folliculitis vs Herpes
Folliculitis is a common skin condition in which hair follicles become inflamed.
The condition presents as small red bumps that may have a white, pus-filled tip. It is most commonly caused by Staph. aureus.
Herpes is a common, life-long infection caused by the herpes simplex virus.
There are two types of herpes viruses: HSV-1 and HSV-2. Both herpes simplex viruses may be transmitted through sex, or by touching or kissing any affected area.
According to the US Centers for Disease Control and Prevention’s National Center for Health Statistics, the prevalence of herpes simplex virus type 1 and HSV-2 is 47.8 percent and 11.9 percent, respectively, for American people aged 14 to 49 years.
READ THIS NEXT:
6 Celebrities With HPV (Human Papillomavirus)
6 Famous People With Avoidant Personality Disorder
Celebrities With Turner Syndrome
9 Famous People With Hemophilia
References https://www.ncbi.nlm.nih.gov/pubmed/23656553 https://onlinelibrary.wiley.com/doi/pdf/10.1111/apm.12103 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3002406/