Alopecia Areata vs Tinea Capitis:
This article reveals the differences between alopecia areata and tinea capitis:
Alopecia Areata (AA)
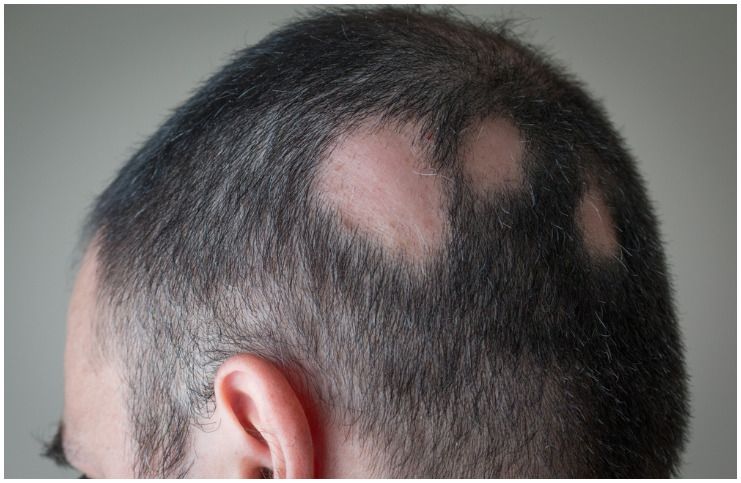
It is a common autoimmune disorder that usually results in unpredictable hair loss. It is most frequent on the scalp, however, it can involve any hair-bearing site, including eyelashes, eyebrows, and beards.
In many cases, the hair re-grows, commonly after a few months. Sometimes, hair loss is permanent.
It affects about 6 million people in the United States, according to the National Alopecia Areata Foundation. Worldwide, it affects up to 2% of the population.
AA strikes both women and men, typically under the age of 20-years old. At least fifty percent of the affected people develop their first patch of hair loss before they are 21.
After androgenetic alopecia and telogen effluvium, AA is the 3rd most common form of hair loss dermatologists see.
Symptoms
Unpredictable hair loss is the only symptom of the disorder.
Complications
People with AA are at higher risk for:
- rheumatoid arthritis;
- inflammatory bowel disease;
- psoriasis;
- lupus;
- atopy – a predisposition toward developing some allergic hypersensitivity reactions, such as – asthma, allergic rhinitis, and atopic dermatitis;
- vitiligo;
- thyroid disease (including Hashimoto’s disease);
- depression;
- anxiety.
Causes
The cause of AA is an autoimmune reaction. This actually means the human body’s immune system attacks its own cells.
Risk Factors
The onset of hair loss is occasionally triggered by:
- physical stressors;
- hormonal change;
- emotional trauma;
- viral infection.
Note – 20 percent of patients with AA have a family member who has experienced the disorder.
Diagnosis

Treatment
For most sufferers, AA resolves without medical treatment within 12 months, however, hair loss is sometimes permanent – for about 10% of patients.
Treatment options include:
- a course of corticosteroids (anti-inflammatory medicines) by mouth or intravenously (for adult patients with extensive hair loss);
- psoralen (a light-sensitive medication that absorbs ultraviolet light) and ultraviolet A phototherapy;
- anthralin (applied to the scalp) – it may stimulate early hair regrowth;
- topical minoxidil (an anti-hypertensive vasodilator medication) – it may stimulate hair growth by increasing the diameter of hairs that start to grow and by accelerating the speed of the natural hair cycle;
- squaric acid dibutyl ester (contact immunotherapy);
- diphenylcyclopropenone (an experimental sensitizing agent);
- cortisone solution injected into the bald patches;
- cortisone cream was applied to the bald patches.
Tinea Capitis
Tinea capitis, also referred to as ringworm of the scalp, is an infection that affects the scalp and hair shafts, leading to small patches of itchy, scaly skin.
Ringworm of the scalp is considered to be a form of superficial dermatophytosis or mycosis. It is most common in toddlers and school-age children. It is endemic in many developing countries.
The estimated prevalence in the US of ringworm of the scalp ranges from 3 to 8 percent. There is an almost equal incidence between the rural and urban populations.
Symptoms
Common symptoms of ringworm of the scalp include:
- painful areas on the scalp;
- fragile hair which easily pulls out;
- patches which have small black dots where the hair has broken off the scalp;
- scaly, gray, or reddened areas;
- patches that slowly enlarge;
- one or more round patches of scaly skin.
Causes
It is caused by an infection with a type of fungus called a dermatophyte. At least 8 species of dermatophytes are associated with the infection.
In the United States, Trichophyton tonsurans is the most common cause, followed by M. audouinii, Microsporum canis, T. violaceum, and T. schoenleinii.
These fungal spores are transmitted through contact with an infected animal or person, contaminated objects, and fallen infected hairs.
READ MORE: Contact Dermatitis vs Scabies
Risk Factors
Risk factors for the infection include:
- use of shared combs;
- hairdressing salons;
- overcrowding (households or schools);
- low immune system;
- emotional stress;
- age (most common in children).
READ MORE: Impetigo vs Herpes
Diagnosis
The diagnosis is confirmed by laboratory studies after taking a sample of skin scales and hairs from the affected areas. In addition, your healthcare professional may use Wood’s lamp, a special light that illuminates the scalp to determine any sign of infection.
Note – the infection may resemble atopic or seborrheic dermatitis and be misdiagnosed for a long time.
Treatment
The usual recommended treatment is an inexpensive oral medication, called griseofulvin, which is taken by mouth for 4 to 6 weeks.
Note – in order to prevent re-infection, all family members and close friends should be checked to make sure they are not carrying the dermatophytes.
READ MORE: Smallpox vs Chickenpox
Alopecia Areata vs Tinea Capitis (Ringworm Of The Scalp) – Differences
Alopecia areata is an autoimmune disease that develops when the immune system mistakes healthy cells for harmful substances. AA produces patches of balding without any precise change in the texture of the affected skin.
Tinea capitis, also known as ringworm of the scalp, is a fungal infection of the scalp and hair shafts that are very common among children throughout the world. The infection is caused by dermatophytes.
READ THIS NEXT: Peyronie’s Disease vs. Normal Curvature
References https://www.ncbi.nlm.nih.gov/pubmed/19881991 https://www.sciencedirect.com/topics/medicine-and-dentistry/tinea-capitis https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3573447/
Interesting