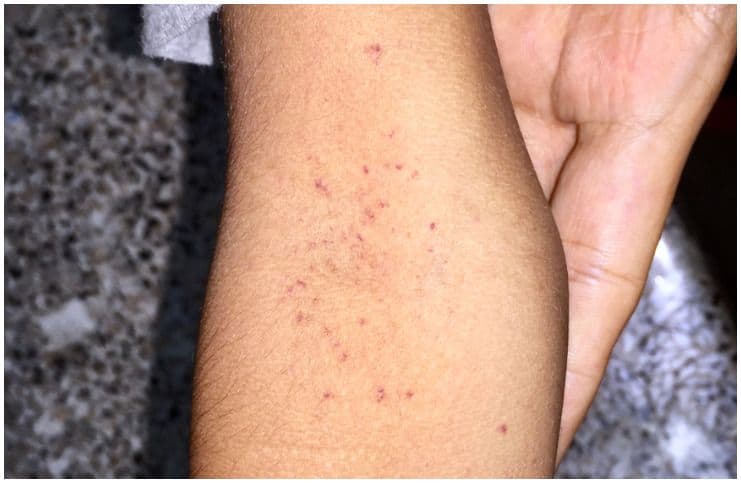
Petechiae vs Purpura – Causes & Differences:
Petechiae
Petechiae are tiny, circular, non-raised patches that appear in a mucous or on the skin or serous membrane.
They commonly appear on your legs, arms, buttocks, and stomach. But, you might find them on your eyelids or inside your mouth.
Petechiae are flush with the surface of the skin and do not blanch under pressure.
Causes
They are formed when tiny blood vessels called capillaries break open.
Certain drugs are linked with the appearance of petechiae. Medications that may cause petechiae as a side effect include:
- sedatives;
- antibiotics;
- nonsteroidal anti-inflammatory drugs;
- heart rhythm drugs;
- blood thinners;
- anti-seizure drugs;
- antidepressants.
Some of the conditions and illnesses which may result in the appearance of petechiae include:
- viral fevers, like – yellow fever, Ebola, and dengue, can inhibit blood clotting, causing bleeding under the skin;
- local trauma or injury causing damage to the skin;
- vasculitis (an inflammation of the blood vessels);
- sunburn;
- scurvy (a disease resulting from a lack of vitamin C);
- allergic reactions to insect bites;
- sepsis;
- various autoimmune diseases;
- a strenuous activity that may cause straining, like – giving birth or lifting weights;
- violent coughing or vomiting;
- bacterial and viral infections;
- bone marrow problems or leukemia which can cause a reduction in the number of platelets;
- medical treatments for cancer, like – chemotherapy or radiation;
- a lower than normal blood platelet level.
Treatment
Assuming there is no underlying medical condition, petechiae commonly resolve themselves within 14 days.
Prevention
There are ways to prevent infections that can cause petechiae:
- if you go outside, check your entire body for ticks when you get back home;
- wash your hands often with water and soap;
- apply an insect repellant containing DEET before you go into grassy or wooded areas;
- practice safe sex;
- clean countertops;
- don’t share utensils, glasses, and other personal items;
- try to stay away from anyone (even friends and family) who appears to be sick.
READ MORE: Cyclothymia vs Dysthymia – Differences
Purpura
It refers to purplish mucosal or cutaneous lesions caused by hemorrhage which occur in mucous membranes or on the skin.
These rashes may bare a closer resemblance to a bruise than a rash. When touched, they may not change colors. Also, they don’t always cause irritation or itch.
There are two common variations of purpura:
- idiopathic thrombocytopenic purpura – it is an autoimmune disease with antibodies detectable against a few platelet surface antigens. ITP can lead to easy or excessive bleeding and bruising.
- Henoch-Schonlein purpura – it results in inflammatory changes in the small blood vessels, and it is the most common form of childhood vascular inflammation. The symptoms of Henoch-Schonlein purpura include the following: kidney involvement, arthritis, digestive tract problems, and a rash.
Symptoms
Common symptoms of this condition include:
- tummy pains;
- spots inside the mouth;
- joint pains;
- feeling under the weather;
- a high temperature (fever);
- tenderness in the area of the rash;
- blisters (that may be yellow or clear like little boils).
Note – the condition is typically self-limited. Hence, treatment is not indicated in all cases, and full recovery is normal.
READ MORE: Chalazion vs Stye (Hordeolum)
Causes
The rash is caused by blood vessels that burst close to the skin’s surface and blood pools. This makes spots visible externally.
Thrombocytopenic purpura may be due to:
- meningococcemia (a bloodstream infection which is caused by the bacterium Neisseria meningitidis);
- immune neonatal thrombocytopenia;
- drugs that reduce the platelet count.
Non-thrombocytopenic purpuras may be due to:
- injury;
- amyloidosis (a disorder in which abnormal proteins build up in organs and tissues);
- certain infections;
- blood clotting disorders;
- steroid use;
- congenital cytomegalovirus (a condition in which an infant is infected with cytomegalovirus);
- scurvy (vitamin C deficiency);
- congenital rubella syndrome;
- pressure changes that occur during vaginal childbirth;
- inflammation of the blood vessels;
- hemangioma (abnormal buildup of blood vessels in the internal organs or skin);
- drugs that affect clotting factors or platelet function.
Risk Factors
Factors that can increase the risk of purpura are:
- advanced age;
- genetics;
- poor blood vessel health;
- blood clotting issues due to disease or medications;
- inflammatory disorders or conditions;
- some types of cancer, such as – myeloma and leukemia;
- poor nutrition;
- infectious disease.
READ MORE: Osteopenia vs Osteomalacia
Bottom Line: Petechiae vs Purpura
Petechiae are round, small reddish or purplish-colored marks or blotches that appear on the skin. The spots can show up all over the body, including places such as inside the mouth or the eyelids. Also, the spots appear in clusters and occur as a result of bleeding under the skin.
Purpura is a condition where an individual has purple-colored blotches or spots on their mucous membranes (like the lining of the nose or mouth) or on their skin. It occurs most frequently in women over age 50. An individual with purpura may have low platelet counts (thrombocytopenic purpuras) or normal platelet counts (non-thrombocytopenic purpuras).
In conclusion, purpura and petechiae can occur from numerous pathophysiologic mechanisms that interfere with the complex process of hemostasis (a process that causes bleeding to stop).
Basically, purpura is a non-blanching spot (a non-blanching spot is one which does not disappear after brief pressure is applied to the area) that measures more than 2 mm, whereas petechiae are pinpoint non-blanching spots that measure less than 2 mm in size. Both affect the mucous membranes and skin.
Note – spots larger than 1 centimeter are called ecchymoses.
READ THIS NEXT: Uveitis vs Iritis
References https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6065062/ http://pediatrics.aappublications.org/content/84/6/1051?maxtosho https://www.sciencedirect.com/topics/medicine-and-dentistry/petechia